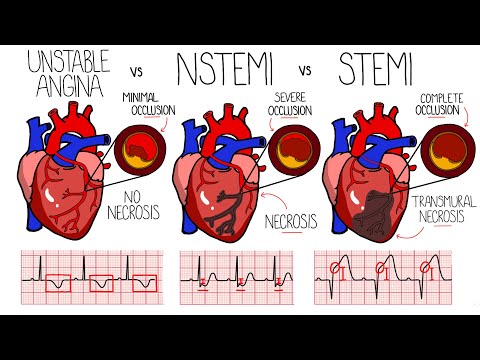
Hey there! So, let’s chat about heart health, shall we? You know how sometimes your chest feels tight or you get that weird pressure? Yeah, that could be angina knocking at your door.
Now, there are two types: stable and unstable angina. Sounds serious, huh? But don’t worry; I’m here to break it down for you. Stable angina is like that annoying friend who shows up but leaves once you rest. Unstable angina? That’s a whole different ballgame—it sticks around and can be a bit scary.
It’s super important to understand these differences. They can help you make sense of what’s going on with your ticker. So grab a cozy seat and let’s dive into the world of stable vs unstable angina!
Effective Treatment Approaches for Stable and Unstable Angina: A Comprehensive Guide
Alright, let’s chat about angina. It sounds fancy, but really, it’s about chest pain that happens when your heart isn’t getting enough blood. There are two types: stable angina and unstable angina. Knowing the difference is key, so grab a comfy seat and let’s break it down!
Stable angina usually pops up during activities that make your heart work harder, like climbing stairs or exercising. And the cool thing? It often goes away with rest or medication. Here’s what you might find helpful:
- Aspirin: This can help thin your blood.
- Nitroglycerin: A quick fix for those sudden flare-ups; it helps relax blood vessels.
- Lifestyle changes: Eating well and exercising can seriously help your heart.
I remember my buddy Sam dealing with stable angina while training for a marathon. He learned to listen to his body and take breaks when needed. This made a huge difference in how he managed his condition.
Now, on to unstable angina. This one’s trickier since it can occur even at rest and doesn’t follow the usual patterns of stable angina. It can be a sign of something more serious brewing in your heart, which means you should definitely see someone who knows their stuff about this! Here are some things associated with unstable angina:
- Noisy symptoms: Pain that suddenly worsens or feels different than before.
- A visit to the doc: More frequent check-ups means keeping an eye on things.
- Meds may change: You might need some stronger prescriptions if you’re dealing with this type.
If we think about it logically, managing both types of angina comes down to understanding your body and working with healthcare pros. They’ll guide you on what feels right for you!
You know what’s crucial? Taking care of your heart isn’t just about pills; it’s also lifestyle! Stress management, having supportive friends (like Sam!), eating healthier meals, and staying active really matter. So don’t forget: always reach out to a doctor when something doesn’t feel right—your health is worth it!
Understanding the 4 E’s of Angina: Key Insights for Heart Health
Angina might sound a bit scary, but understanding it doesn’t have to be! Basically, angina is chest pain or discomfort that happens when your heart doesn’t get enough blood. It’s like your heart is raising its hand saying, “Hey, I could use a little more oxygen over here!” Let’s break it down into four key insights to help you grasp the basics of angina.
1. The Difference Between Stable and Unstable Angina: Stable angina tends to pop up during physical activity or stress. It’s predictable and usually goes away with rest or medication. Imagine you’re climbing a flight of stairs and feeling that tightness in your chest—it fades when you chill out for a minute. On the other hand, unstable angina is more unpredictable and can occur even at rest. This type can last longer and might signal something more severe going on with your heart.
2. Symptoms to Recognize: Symptoms can vary from person to person, but there are some common signs you might experience with both types of angina:
- Pain or discomfort in the chest
- Pain that radiates to arms, neck, jaw, or back
- Shortness of breath
- Nausea or fatigue
It’s essential to pay attention if these symptoms change or worsen.
3. Causes Behind Angina: So what causes this? It’s usually due to narrowed arteries from conditions like coronary artery disease. That’s where fatty buildups—called plaques—block blood flow. Imagine trying to squeeze toothpaste out of a tube: if the opening is partially blocked, it takes effort! The same goes for your arteries; when they’re narrowed, your heart has to work harder.
4. Seeking Help: If you experience any symptoms that worry you, reaching out to a healthcare professional is super important! They can help figure out what’s going on and discuss potential solutions tailored just for you.
Understanding these four points about angina makes navigating heart health less daunting! Remember that while it’s helpful to know about symptoms and causes, nothing beats professional healthcare advice when it comes down to it. Keep your heart healthy by staying informed and proactive!
Stable vs. Unstable Angina: Understanding the Severity and Implications for Heart Health
Okay, let’s talk about angina. It sounds a little scary, right? But it’s just a term used to describe chest pain or discomfort that comes from the heart not getting enough blood. There are two main types: stable angina and unstable angina. Knowing the difference is super important for heart health.
Stable angina usually hits when you’re doing something physical or feeling stressed. You know, like when you’re climbing a hill or running to catch the bus? It’s often predictable and goes away with rest or medication quite quickly. Think of it like your heart saying “Hey, slow down a bit!” So, in these moments, it’s kind of your body’s way of helping you out.
On the other hand, unstable angina is more serious and can strike unexpectedly. This one might happen while you’re just chilling on your couch or even while sleeping! This type can last longer and doesn’t go away easily with rest or regular meds. It’s like your body yelling “Red alert!”—so it requires immediate attention.
- Symptoms of stable angina:
- Pain during physical activity
- Pain relieved by resting
- Symptoms of unstable angina:
- Pain at rest
- Pain lasting longer than usual
- Pain that’s more intense than before
You know what really hits home for me? My friend Mark had stable angina for years. He learned to manage it well until one day he had an episode that felt way different—way scarier! Turns out it was unstable angina, and he had to go see someone right away. That moment taught him how crucial it is to stay aware and keep communication open about his heart health.
The bottom line is this: if you experience chest pain, don’t ignore it! Recognizing whether it’s stable or unstable can make all the difference in getting the right help. Always chat with a healthcare professional about any concerns—seriously, they got your back!
Your heart’s well-being matters, so keep an eye on those signals!
Understanding the Pathophysiology of Stable vs Unstable Angina: Key Differences and Implications
Hey there! Let’s chat about something that affects a lot of people: angina. It’s like a warning signal from your heart saying, “Hey, I might need some help here!” There are two main types—stable angina and unstable angina. Understanding the differences between them can really help you appreciate what’s going on in your body.
Stable angina is kind of predictable. It usually happens when you’re doing something physical, like climbing stairs or running. Your heart needs more oxygen during those times, and if it can’t get it because of narrowed arteries, you might feel that familiar chest pain or discomfort. The good news? It goes away with rest or medication.
Now, unstable angina, well, that’s a different beast altogether. This one can strike out of the blue, even while you’re just chilling on the couch. It might last longer and be more intense than stable angina too. This situation is trickier because it could be a sign that a heart attack might happen soon.
- Causes: Both types arise from reduced blood flow due to narrowed arteries caused by plaque buildup, but the key difference is stability and predictability.
- Symptoms: With stable angina, you’ll likely feel pain during exertion; unstable can surprise you anytime with severe discomfort.
- Treatment: Stable is often managed with lifestyle changes and medication, while unstable may require more urgent medical care.
I remember my friend Tom who experienced stable angina when he was hiking. He knew to take breaks and rest when it hit him because he understood his body’s signals. But then one day at work, he felt that unmistakable pain without any warning—it turned out to be unstable angina! Fortunately, he got checked out right away. Crazy how quickly things can change!
The bottom line is understanding these differences isn’t just about knowing the terms; it’s about recognizing what your body is telling you. If anything feels off or different, reaching out to a healthcare professional is always the best bet!
Your heart health matters—take care of it! And remember, this info doesn’t replace professional healthcare advice.
So, let’s chat about angina for a sec. It might sound fancy, but it’s really just a way to describe chest pain that comes from the heart not getting enough blood. There are two main types: stable and unstable. And trust me, they’re different in some pretty significant ways.
First up is stable angina. Picture this: you’re out for a jog or maybe climbing a flight of stairs—your heart starts racing and that familiar pressure or pain kicks in. But here’s the thing: it usually goes away after you rest or slow down. It’s like your heart’s little warning light saying, “Hey, chill for a minute!” It’s predictable too; you can kind of expect when it’ll pop up.
Now, on the other hand, unstable angina is a whole different ball game. Imagine walking to the fridge for a snack—nothing too intense—and suddenly you feel that tightness in your chest outta nowhere and it doesn’t go away easily. It could even happen when you’re just hanging out on the couch! That’s scary stuff because it can signal something more serious going on with your heart.
You know, I once had this friend who thought he was just dealing with “normal” stress levels at work, which led to occasional chest pain after long hours. He shrugged it off as typical until one day he found himself struggling to breathe after some light lifting. Turned out he had unstable angina and needed medical attention ASAP! It was a wake-up call for everyone around him.
When navigating these two types of angina, it’s really important to keep an eye on how you’re feeling day-to-day—like truly listen to your body. Stable might be annoying but manageable; unstable? Well now, that’s definitely an urge to seek help right away! Always remember that professional healthcare advice is key—you wanna make sure you’re getting the right support if things start feeling off.
So anyway, if you ever find yourself feeling those symptoms or have questions swirling in your mind after reading about these types of angina, don’t hesitate to chat with someone who knows their stuff. Your heart’s health is super important and getting clarity can make all the difference!
